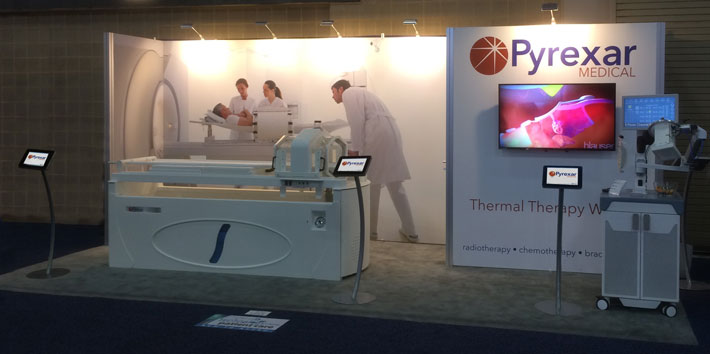
Our distributor in Spain invited Mark Falkowski, CEO of Pyrexar, to participate in a conference sponsored by the Spanish Societies of Radiation Oncology (SEOR) Hyperthermia Group. Oncologists from the area converged in Málaga, Spain, to talk about a new type of adjunct cancer treatment. They gathered to learn about the positive clinical trials and growing success that surrounds a specific type of thermal therapy, rf (radio frequency) hyperthermia. Energy is directed deep into the body then focused and steered by adjusting wave frequency and amplitude, resulting in targeted “fever”
Our distributor in Spain invited Mark Falkowski, CEO of Pyrexar, to participate in a conference sponsored by the Spanish Societies of Radiation Oncology (SEOR) Hyperthermia Group. Oncologists from the area converged in Málaga, Spain, to talk about a new type of adjunct cancer treatment. They gathered to learn about the positive clinical trials and growing success that surrounds a specific type of thermal therapy, rf (radio frequency) hyperthermia. Energy is directed deep into the body then focused and steered by adjusting wave frequency and amplitude, resulting in targeted “fever”  temperature (41-42C) at the tumor site. Heat sensitizes and improves blood flow at the tumor site, which, in turn, increases the amount of chemotherapy that reaches inside the tumor. Blood flow also brings oxygen to these hypoxic (without oxygen) cancer tumors, increasing the effectiveness of radiation therapy. Phase 3 clinical studies demonstrate that hyperthermia, along with chemotherapy or radiotherapy, increases tumor control of up to 300% when compared to radiotherapy or chemotherapy alone.
temperature (41-42C) at the tumor site. Heat sensitizes and improves blood flow at the tumor site, which, in turn, increases the amount of chemotherapy that reaches inside the tumor. Blood flow also brings oxygen to these hypoxic (without oxygen) cancer tumors, increasing the effectiveness of radiation therapy. Phase 3 clinical studies demonstrate that hyperthermia, along with chemotherapy or radiotherapy, increases tumor control of up to 300% when compared to radiotherapy or chemotherapy alone.
 Thanks to regional groups like the SEOR and companies like Magna Medic, this newest cancer fighter will be available in the near future. “Facilities, like Clínica Ruber Internacional (Madrid), Vithas Xanit International Hospital (Málaga), Instituto Valenciano de Oncología (Valencia) and Centro Médico Teknon (Barcelona)” are the types of progressive institutions that look for cancer treatment innovations,” says Felix Navarro, Medical Physicist at the Magna Clinic Marbella, “We are very experienced with hyperthermia in our clinic, and we look forward to sharing our successes with the country.”
Thanks to regional groups like the SEOR and companies like Magna Medic, this newest cancer fighter will be available in the near future. “Facilities, like Clínica Ruber Internacional (Madrid), Vithas Xanit International Hospital (Málaga), Instituto Valenciano de Oncología (Valencia) and Centro Médico Teknon (Barcelona)” are the types of progressive institutions that look for cancer treatment innovations,” says Felix Navarro, Medical Physicist at the Magna Clinic Marbella, “We are very experienced with hyperthermia in our clinic, and we look forward to sharing our successes with the country.”
In preparation for the expected technology growth in hyperthermia cancer treatment sector, Magna Medic has signed a six year, $3 million (USD) distribution contract with hyperthermia device maker Pyrexar Medical. “We are excited to see cancer patients get the treatment they deserve,” says Mark Falkowski, Pyrexar CEO, “and we could not find a more capable partner than Magna Medic.”

 We had a great week in Dubai at the Arab Health show. Dubai is the most populous city in the United Arab Emirates (UAE), located on the southeast coast of the Persian Gulf and is one of the seven emirates that make up the country. The 2016 exhibition showcased more than 4,000 companies exhibiting their latest innovations to more than 130,000 healthcare professionals attending from 163 countries.
We had a great week in Dubai at the Arab Health show. Dubai is the most populous city in the United Arab Emirates (UAE), located on the southeast coast of the Persian Gulf and is one of the seven emirates that make up the country. The 2016 exhibition showcased more than 4,000 companies exhibiting their latest innovations to more than 130,000 healthcare professionals attending from 163 countries.
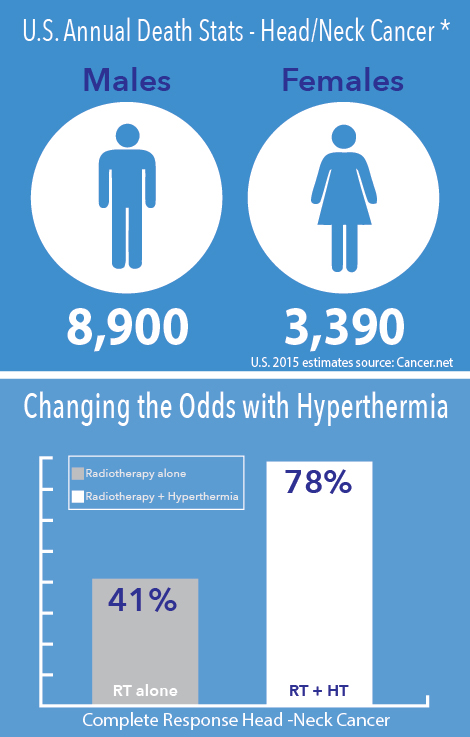 Published last month in the
Published last month in the 

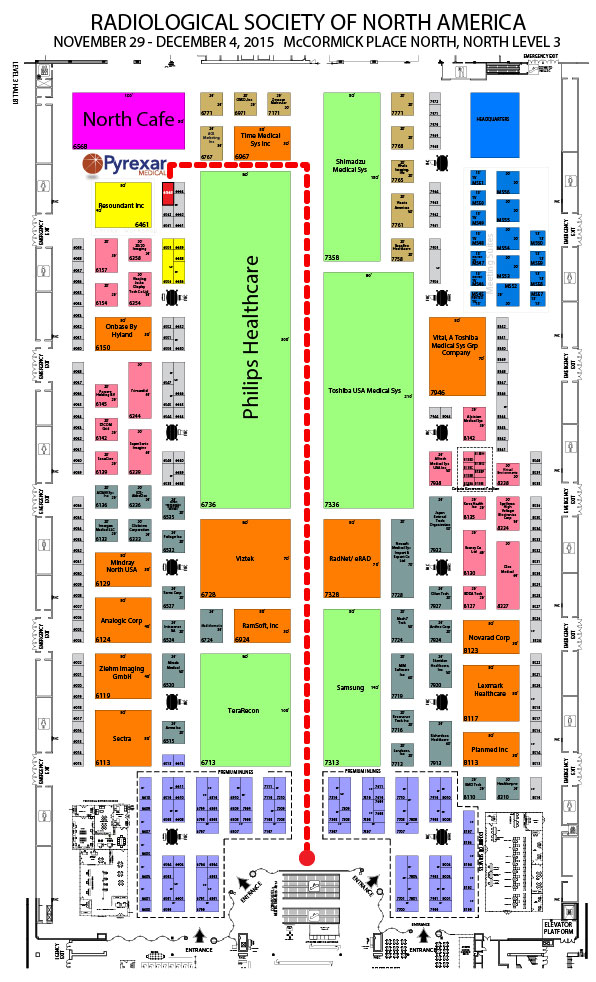 This year the
This year the